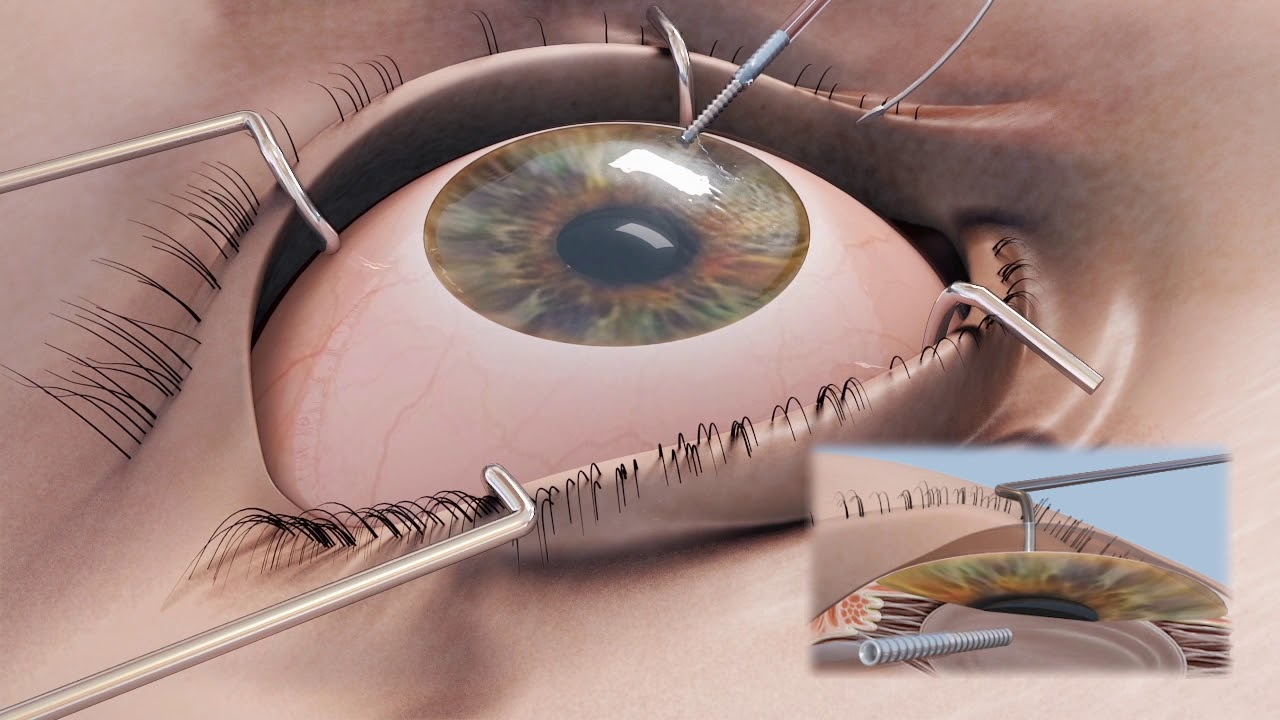
Corneal repair surgery has emerged as a groundbreaking solution for individuals suffering from severe corneal damage that traditional treatments cannot rectify. At Mass Eye and Ear, this innovative approach utilizes stem cell therapy as a means to restore the cornea’s surface, offering renewed hope for those facing blinding eye injuries. The procedure, known as cultivated autologous limbal epithelial cells (CALEC), involves harvesting limbal epithelial cells from a healthy eye, cultivating them, and then transplanting them back into the damaged eye. Clinical trials have shown remarkable progress in restoring vision and alleviating pain, making corneal repair surgery a beacon of possibility for patients who previously had no viable options. By implementing cutting-edge techniques and extensive research, this method exemplifies a significant leap in eye injury treatment, paving the way for more effective corneal transplant outcomes in the future.
Exploring the realm of ocular rehabilitation, corneal restoration surgery represents a pivotal advancement in the management of serious eye damage. This innovative process, often referred to as regenerative eye surgery, harnesses the power of stem cell technology to mend the eye’s transparent layer—the cornea. Utilizing harvested limbal epithelial cells, this treatment efficiently restores the corneal surface, effectively addressing issues arising from traumatic injuries and chronic conditions. As research progresses, similar techniques, including potential allogeneic methods, could widen the scope of eye injury treatment, making it accessible to a broader range of patients. The collaborative efforts at Institutions like Mass Eye and Ear signify a commitment to revolutionizing ophthalmic care through sophisticated methodologies and dedicated clinical trials.
Understanding Corneal Repair Surgery
Corneal repair surgery is a pivotal advancement in ophthalmology, particularly for patients suffering from debilitating eye injuries or conditions that impair their vision. This type of surgery aims to restore the integrity of the cornea, the outermost layer of the eye, which is crucial for light entry and vision clarity. One innovative approach within this field is Cultivated Autologous Limbal Epithelial Cells (CALEC) surgery. This technique focuses on utilizing stem cells harvested from a healthy eye to regenerate the damaged corneal surface, representing a significant breakthrough for individuals who previously faced limited treatment options.
Prior to advancements like CALEC, corneal transplant surgery was often the only recourse for patients with severe corneal damage. The limitations of corneal transplants, such as the need for a compatible donor and the risks associated with surgery, have propelled research into alternative therapies. Recent studies, particularly at Mass Eye and Ear, have highlighted that stem cell therapy not only provides a new method of repairing eye injuries but also boasts impressive success rates, with over 90% efficacy in restoring corneal surfaces. This innovation shines a hopeful light on future treatment pathways for ocular health.
The Role of Stem Cell Therapy in Eye Injuries
Stem cell therapy has revolutionized the treatment landscape for eye injuries, particularly those affecting the cornea, which is essential for maintaining vision. By employing stem cells—specifically limbal epithelial cells—from a healthy eye, surgeons can create grafts that are transplanted into areas where the cornea has been damaged. This process helps regenerate the corneal surface, restoring both function and aesthetics. At Mass Eye and Ear, clinical trials have successfully demonstrated the safety and efficacy of this approach, making stem cell therapy a promising option for tackling eye injuries that were once deemed irreparable.
Incorporating therapies like CALEC into clinical practice addresses a critical gap in traditional eye injury treatment. Whereas standard methods often fall short for patients with extensive corneal damage, stem cell techniques offer a new avenue for regeneration. These developments underscore the importance of research collaborations, such as those observed between Mass Eye and Ear and leading institutions like Dana-Farber, which are pivotal in advancing stem cell applications in ocular therapy. As ongoing studies continue to explore larger populations, the hope is to establish widespread treatment strategies that can accommodate various degrees of eye injury.
The Importance of Limbal Epithelial Cells in Corneal Health
Limbal epithelial cells play a vital role in maintaining the health and function of the cornea. These specialized cells are located at the limbus, the border between the cornea and the sclera, and are crucial for ensuring a stable, transparent corneal surface. When these cells are compromised due to injury or disease, the cornea cannot heal effectively, which can lead to vision impairment and discomfort. Understanding the significance of limb cells highlights the need for advanced repair methods, such as stem cell therapy and corneal repair surgery, to restore normal functioning.
Recent advancements in the cultivation and application of limbal epithelial cells have enabled surgeons to approach corneal injuries with renewed optimism. By utilizing a patient’s own cells to regenerate damaged areas, the risk of rejection is minimized, which is a significant concern with traditional corneal transplants. This personalized approach not only enhances safety but also improves the likelihood of a successful recovery. Such innovative techniques as CALEC surgery create new prospects for patients who experience a limbal stem cell deficiency, positioning them for potential recovery and improved quality of life.
Exploring Corneal Transplant Alternatives
While corneal transplants have been a cornerstone of treatment for severe corneal damage, they are not without their limitations, including donor availability and the risk of rejection. Alternatives like stem cell therapies are emerging as viable options for restoring vision in patients who do not qualify for traditional transplantation. The CALEC method, developed at Mass Eye and Ear, exemplifies this shift, showcasing the potential of regenerative medicine to address corneal injuries with impressive safety and efficacy.
Through methods like CALEC, patients who face limbal stem cell deficiencies can experience significant improvements in their corneal health. As research progresses, the development of more accessible treatment options for those with corneal damage may help alleviate the burden on the healthcare system and enhance patient outcomes. Additionally, transitioning from donor-dependent treatments to self-sustainable therapies offers promising pathways in the field of ocular health, making it imperative to continue funding and researching innovative approaches.
Clinical Trials: Pioneering Eye Injury Treatments
Clinical trials are essential in advancing new treatment protocols for eye injuries and ensuring that innovative therapies reach those who need them most. The groundbreaking work on CALEC at Mass Eye and Ear represents a significant milestone in the journey towards effective eye injury treatment using stem cell technology. Over the course of the trial, researchers have collected valuable data that reflect not only the safety of the treatment but also its high success rate in restoring corneal surfaces, reaffirming the potential of such therapies in clinical settings.
The meticulous process of conducting clinical trials for stem cell therapies involves multiple layers of regulatory scrutiny, including oversight from the U.S. Food and Drug Administration. This rigorous evaluation ensures that any new treatment, including those based on limbal epithelial cells, adheres to the highest safety and effectiveness standards before being adopted into common practice. As shown by the promising results from ongoing clinical trials, the emergence of these therapies could eventually reshape the paradigms for treating severe ocular injuries and conditions, giving many individuals the chance to recover their vision.
Future Directions for Eye Injury Treatments
As research in the field of ophthalmology advances, future directions for treating eye injuries center on improving stem cell therapies and expanding their accessibility. For example, the development of allogeneic manufacturing processes for CALEC could broaden the treatment spectrum, allowing patients with damage in both eyes to benefit from stem cell interventions. Such innovations are crucial as they could potentially treat a larger demographic, offering new hope for many who currently have limited options due to the necessity of a healthy donor eye.
Moreover, the future of eye injury treatments hinges on comprehensive studies that involve larger patient cohorts across multiple centers. By conducting larger-scale research with randomized-controlled designs, researchers can garner more robust data to support the efficacy of these treatments. Continuous collaboration among institutions like Mass Eye and Ear, Dana-Farber, and others is vital to push the boundaries of what is currently known about corneal repair and injury management, ultimately leading to transformative change in patient care strategies.
Safety Profiles of Corneal Repair Techniques
Understanding the safety profile of corneal repair techniques, particularly in the context of stem cell therapies, is paramount for clinicians and patients alike. The initial trials of CALEC have shown a high safety profile, with minimal adverse effects reported during patient recovery. This data underscores the potential for using cultivated limbal epithelial cells as a secure method for treating severe corneal injuries, highlighting the importance of ongoing monitoring and evaluation to solidify these findings.
In addition to safety, the long-term outcomes of such treatments must be assessed to ensure their viability as standard care options. Analyzing how patients fare over months and years post-treatment will provide insights into the durability of the corneal repairs achieved through stem cell intervention. As researchers continue to refine these practices and understand the implications of their findings, the goal remains to develop treatment protocols that prioritize patient safety while delivering effective care.
The Cost of Corneal Repair Treatments
The cost of corneal repair treatments, including innovations like CALEC, can be a concern for many patients and healthcare providers. While stem cell therapy offers promising outcomes, financial considerations play a significant role in determining accessibility. In order to ensure that these advanced treatments become widely available, public and private funding, insurance coverage policies, and healthcare system support will need to evolve alongside these medical breakthroughs, facilitating better access for patients in need.
It’s also important to consider the economic impact of advancing corneal repair methods. By investing in innovative treatments that can prevent or heal blindness caused by corneal injuries, healthcare systems may ultimately reduce the long-term costs associated with managing chronic eye disease. Promoting early interventions through therapies such as CALEC not only enhances patient quality of life but could also lead to substantial cost savings for both families and healthcare providers.
Significant Collaborations Enhancing Ocular Research
Collaborations among leading research institutions play an instrumental role in the evolution of ocular research and treatment methodologies. By working together—like Mass Eye and Ear’s partnership with Dana-Farber—scientists can share insights, resources, and expertise to drive forward the development of groundbreaking treatments such as CALEC. This teamwork is crucial in the intricate field of stem cell therapy, where interdisciplinary approaches can unveil new solutions for complex issues like eye injuries.
The result of effective collaborations leads to comprehensive clinical trials and thorough investigations, which bolster the credibility of emerging treatments. As researchers pool their knowledge and experience, they not only enhance the prospects of success for new therapies but also pave the way for innovative applications that can transform the field of ophthalmology. Ultimately, these partnerships exemplify the collective commitment of the medical community to advance patient care and expand treatment horizons for eye injury management.
Frequently Asked Questions
What is corneal repair surgery and how does it help with eye injuries?
Cornel repair surgery, including the innovative stem cell therapy known as cultivated autologous limbal epithelial cells (CALEC), addresses severe corneal damage from injuries such as chemical burns or infections. This procedure restores the cornea’s surface by transplanting healthy limbal epithelial cells harvested from a patient’s unaffected eye, significantly improving vision and quality of life for those with previously untreatable conditions.
How does stem cell therapy in corneal repair surgery work?
Stem cell therapy in corneal repair surgery involves extracting limbal epithelial cells from a healthy eye, expanding them in a laboratory to create a tissue graft, and then transplanting this graft into the damaged eye. This technique, developed at Mass Eye and Ear, has demonstrated over 90% effectiveness in restoring corneal integrity and function, providing new hope to patients with significant corneal injuries.
What types of corneal injuries can be treated with corneal repair surgery?
Corneal repair surgery can address various corneal injuries, including those caused by chemical burns, trauma, or infections that lead to limbal stem cell deficiency. This deficiency prevents natural regeneration of the cornea, making innovative treatments like CALEC essential for restoring a functional ocular surface.
Is corneal transplant the standard treatment for corneal damage, and how does CALEC compare?
Corneal transplant is a common treatment for severe corneal damage; however, it may not be suitable for patients with limbal stem cell deficiency. In contrast, CALEC, a novel approach at Mass Eye and Ear, offers a regenerative treatment option by restoring corneal surfaces using the patient’s own stem cells, resulting in a higher success rate for those who cannot undergo traditional transplants.
What are the potential outcomes of undergoing corneal repair surgery with CALEC?
Clinical trials have shown that corneal repair surgery using CALEC resulted in significant improvements, with 50% of participants achieving complete corneal restoration by three months, and success rates increasing to 79% and 77% at 12 and 18 months, respectively. These outcomes highlight CALEC’s potential in effectively treating severe corneal injuries.
Are there any risks associated with CALEC surgery for corneal repair?
While CALEC surgery for corneal repair has demonstrated a high safety profile in clinical trials, there are still potential risks. Minor adverse events have been observed, such as infections related to improper contact lens use. Overall, serious complications were rare, emphasizing the need for careful patient selection and follow-up.
Is CALEC therapy available for patients today, and what does the future hold?
Currently, CALEC therapy remains experimental and is not yet widely available, as additional studies are needed before it can be submitted for FDA approval. Future research aims to include larger patient groups and potentially establish allogeneic manufacturing processes to treat individuals with damage to both eyes at facilities like Mass Eye and Ear.
What role do limbal epithelial cells play in corneal health and repair?
Limbal epithelial cells are essential for maintaining the cornea’s smooth surface and overall health. When damaged, these cells cannot regenerate on their own, leading to conditions like limbal stem cell deficiency. Innovative procedures like CALEC surgery utilize these cells to restore the corneal surface and improve vision in affected patients.
Who conducted the first CALEC surgery and what were the results?
The first CALEC surgery was performed by Ula Jurkunas at Mass Eye and Ear, yielding promising results in clinical trials. The procedure safely restored corneal surfaces in 14 patients over an 18-month follow-up, demonstrating its effectiveness and paves the way for future treatments of corneal injuries.
What are the clinical trial results for CALEC as a corneal repair surgery option?
Clinical trials of CALEC have shown remarkable results, with a 93% overall success rate in restoring corneal surfaces among participants. The safety profile was also positive, with no serious adverse events during the follow-up period, making CALEC a promising option for those facing severe corneal damage.
| Key Point | Details |
|---|---|
| Overview of CALEC Surgery | The CALEC surgery involves taking stem cells from a healthy eye and transplanting them into a damaged eye to restore the cornea’s surface. |
| Clinical Trial Success | In a trial involving 14 patients, the treatment showed over 90% effectiveness in restoring corneal surfaces after 18 months. |
| Procedure Details | Stem cells are harvested from a healthy eye, expanded into a graft, and then surgically transplanted into the damaged eye. |
| Safety Profile | The procedure has a high safety profile with no serious adverse events reported during the trial. |
| Future Prospects | Plans to use allogeneic limbal stem cells from donors could expand treatment possibilities for patients with damage in both eyes. |
Summary
CORNEAL REPAIR SURGERY has made significant advances with the introduction of CALEC (cultivated autologous limbal epithelial cells) treatment. This innovative approach offers new hope for patients suffering from blinding corneal injuries, proving effective in restoring corneal surfaces in clinical trials. As researchers continue to refine this technique and address current limitations, the future of CORNEAL REPAIR SURGERY looks promising, potentially transforming the landscape of treatment options for those with corneal damage.